The frustrating initial medical encounter commonly goes like this:
Doctor: “Hello Ms. Jones, how can I help you?”
Ms. Jones: “Doctor, I have been suffering with terrible migraines”
Doctor: “Based on your description, I think you are suffering with migraines.”
Ms. Jones to herself: (I told YOU that)
Doctor: “Let’s get an MRI of your brain and EEG and some basic lab tests and I will see you in 2 weeks.”
Follow up visit
Doctor: “Ms. Smith, good news is that the MRI and EEG are normal”
Ms. Jones to herself: (so why am I in constant pain?)
Ms. Jones: “That’s good”
Doctor: “I am going to start you on X medication. Come back and see me in a few weeks. Don’t worry, if that doesn’t work, I will give you Y medication. If that doesn’t work, I will give you an anti-seizure medication called Topamax. And, if that doesn’t work, we can do 31 Botox injections in your scalp every 3 months or cut the nerves at the base of your head.”
Although this scenario is common, it is not normal. We can do better.
I’ve been treating and researching migraine for years. What I’ve found is that most of the research about migraine actually already exists. However, for some reason no one had put all the different research together and come up with an overall explanation or treatment for migraine.
Based on my research and experience, I’ve simplified the explanation of migraine to these 4 main Pillars:
- Metabolic
- Nutritional
- Musculoskeletal
- Neurological
True Migraine has been shown to have a genetic predisposition. It is an altered brain state that occurs when the stress of these 4 pillars becomes too much.
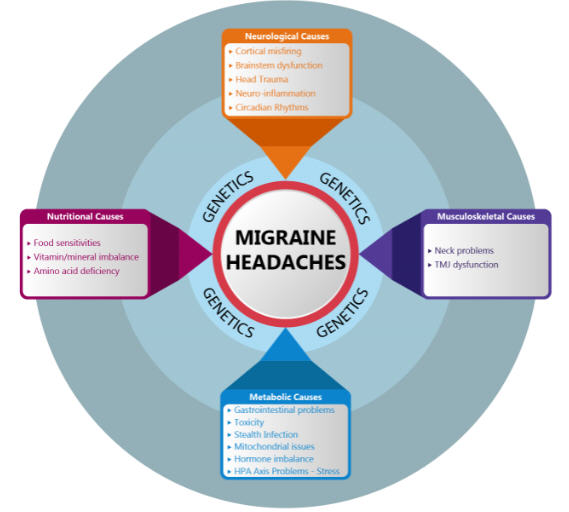
Our goal is to identify things that are not working appropriately with these 4 areas. When we find them, we fix them. Most of the time, a migraine patient has too much of something and not enough of something else. These imbalances do not allow the brain to fire appropriately and the end result is pain, dizziness, visual changes, etc.
Addressing the 4th factor, the Neurological factor, is how we expand someone’s neurological resilience. We examine to identify the part of the brain that is causing migraine to occur in your case, and provide specific, customized brain therapies to strengthen this area. This allows you to be able to handle a higher amount of stress before a migraine occurs.
By also addressing the biochemical, nutritional and musculoskeletal issues, we are able to correct all 4 factors of migraine and push you as far down the migraine spectrum as possible. With most patients, we see the intensity and frequency of migraine diminish significantly.
1. The Metabolic Factor
Your brain swims in a soup of biochemicals that influence the way it works on a regular basis. It is extremely sensitive to toxins and changes in nutrient levels.
For example, you probably drink about 50-100 oz. of water each day. But if you had 3 oz. of vodka without eating, your brain would feel immediate effects! Imagine if you were exposed to tiny amounts of toxins over a long period that built up in your system?
How about your hormones! These chemicals change on a regular basis and also directly impact brain function. Many female patients report that they have a flare up in symptoms around the beginning of their cycle, which is why estrogen is often prescribed. I find that estrogen being low or needing to be supplemented is usually part of a bigger problem. This is why we prefer to take a ‘top down’ approach when looking at hormones and also run a comprehensive hormonal panel to see what might be causing the issues. While hormones don’t cause migraine, they play a big role and will make someone much more likely to have a migraine if they are dysfunctional.
We also know that the intestinal system plays a direct role in brain function. We have trillions of bacteria in the gut that are constantly producing chemicals that change how we think and feel, influence our immune function, produce vitamins and even communicate directly with the brain. With so many people having issues with digestion, IBS and reflux, there is often an overlap with migraine symptoms.
2. The Nutritional Factor
A healthy diet and removal of common ‘triggers’ is essential for proper migraine treatment. However, many of my patients have tried just about every diet for migraine and will report that they didn’t help out. This is much more common than you would expect. This is why it’s important to understand that nutritional changes won’t cause or cure migraine, but they are a piece of the puzzle. Some patients have an extreme response to certain foods, histamine responses and/or cross-reactivities, so making these seemingly simple changes may drastically improve their migraine days and intensity. However, if dietary triggers aren’t a big contributor to another patient, they can try every diet and supplement under the sun without seeing much of a change. This is why we focus on not only looking at the current research on migraine and diet, but also blood sugar and other common factors that make people more likely to avoid migraine. Some patients have such a significant dietary contribution to their migraine syndrome that nutritional changes can set the stage for significant foundational changes in brain function.
3. The Musculoskeletal Factor
Any increased physical stress on the body will make a person more likely to have migraine. This is why the research shows positive outcomes for migraine with almost any body work type of therapy. There is good research for massage, acupuncture, chiropractic, and exercise. These are all great modalities, but the one thing they have in common is that they reduce the amount of musculoskeletal stress on the system.
The brain needs activation and this comes through our senses. Powerful brain stimulation occurs when the muscles and joints are mobilized. This is why a thorough functional examination is so important to understanding which modality will be most beneficial. Structural work on the neck and jaw often help our patients.
4. The Neurological Factor
The neurological component has 2 aspects to consider. The first is the genetic predisposition to migraine. Migraineurs have an altered brain state that is different from people that don’t have migraine, even when they are not having any symptoms. The way this seems to present is through certain regions of brain cells become more likely to fatigue or fail, leading to symptoms associated with migraine.
For example, if your genetic predisposition is in an area associated with pain inhibition of the face, and that area fails, you’ll experience a migraine. If your predisposition is in the area associated with sight, you’ll have visual symptoms. If it is in the area associated with balance, you can experience dizziness. The underlying pathology is basically the same, it just impacts different parts of the brain and brainstem. Therefore, the basic idea behind the neurological component is to identify the areas of the brain that are functionally not as healthy as the others, and stimulate that part of the brain at an appropriate level. Too much stimulation can actually lead to a migraine, and too little won’t make much of an impact. This is why we use a graduated approach in which some people will be given a great amount of stimulation right away, and some get very little. The key is to continually strengthen these parts of the brain, and essentially train the brain with neuro exercises.
The other aspect of the brain has to do with injury and general neurological dysfunction. It is very common, for example, to see someone who gets in a car accident or has had a concussion to have a noticeable increase in migraines. It’s not that these injuries caused migraine, but the stress on the brain and nervous system makes them more likely to have migraine. This can also happen with vestibular imbalances, difficulty with eye or head movements, or difficulty with motion. Improving any of these aspects will help move you down the spectrum of migraine to have less and less.
Very often, we discover that patients with migraines have head trauma or concussions in the past and never connected the two. People erroneously think that if they are not knocked unconscious, that a blow to the head can cause long term issues.